How to Determine Osseointegration Before Final Restoration
Jun 3, 2016
Have you ever placed an implant in an augmented bone site and added another few months of healing time just to be on the safe side?
Requests for shorter treatment times along with a growing number of patients with risk factors place greater demands on dentists and the available technology. There is an increasing need to evaluate implant stability before final restoration that cannot be achieved using traditional methods such as torque and percussion tests.
It has long been recognized in the dental implant industry that implant stability is a critical factor in predictable treatment outcomes. Implant stability can be expressed as the absence of micro mobility, meaning the implant’s potential to move on a microscopic level. That is, the more stable the implant is the less micro mobility there will be. Too much micro motion can damage the healing process. Some of the other factors to consider include bone quantity and quality, patient risk factors and experience level of the surgeon.
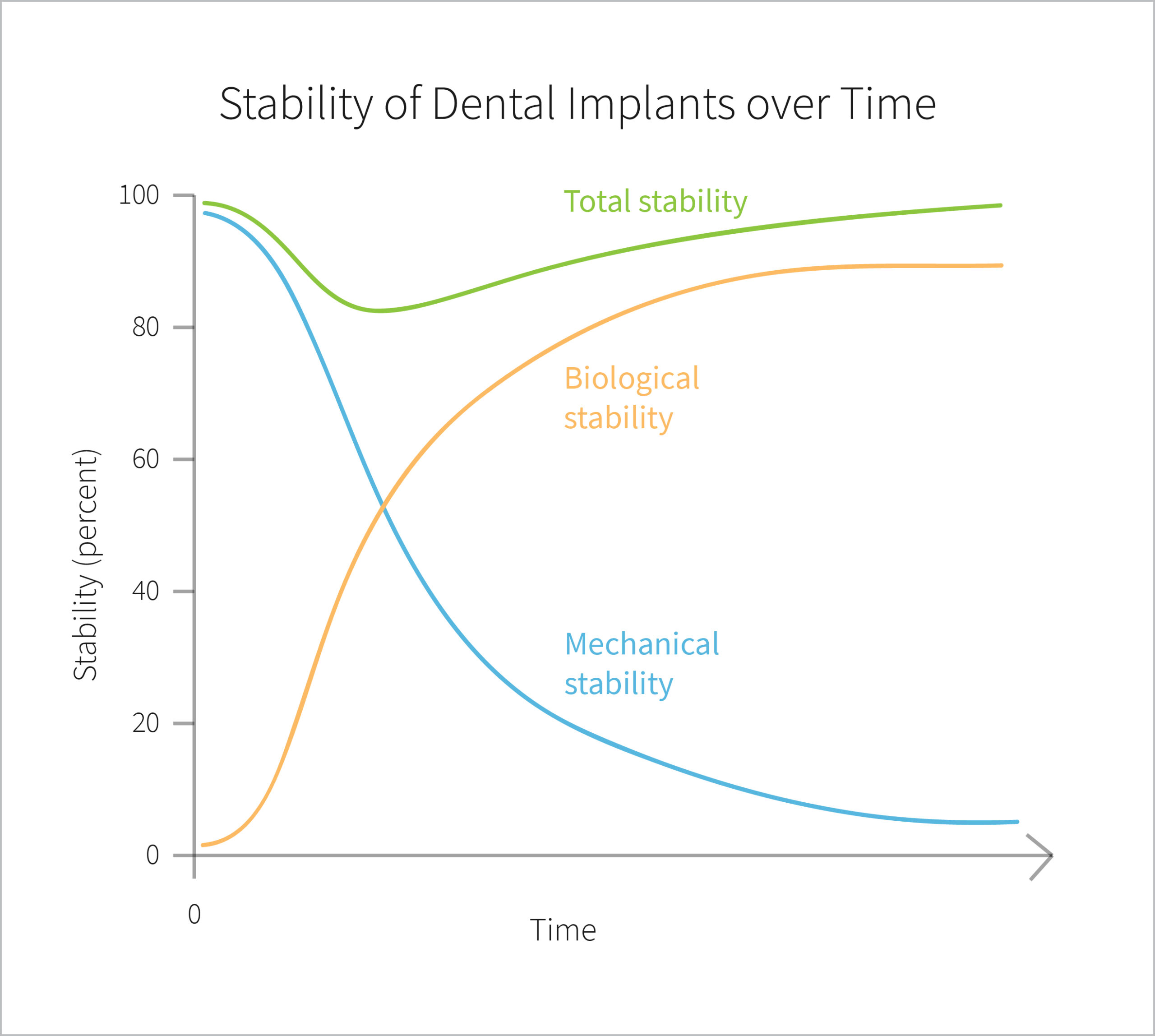
At implant placement the stability consists only of mechanical stability. This will decrease with time and be replaced by biological stability, also known as osseointegration. For the treatment to be successful the stability level needs to be high enough both at implant placement and in the long run, thus the development of osseointegration is key.
Osseointegration normally starts to show in a couple of weeks after implant placement and can be measured at patient check-ups. This will ensure that the stability level is high enough before the implant is loaded with the final restoration.
There are several methods to measure primary implant stability. The most commonly used are RFA (Resonance Frequency Analysis), tactile feeling, torque test, and percussion test. However, RFA is the only objective, non-invasive and repeatable way to measure the degree of osseointegration before final restoration – allowing you to determine the optimal loading time, and thereby potentially reducing treatment times and avoiding premature loading.